Blount’s Disease
Jeanne Franzone, M.D.
Introduction
Blount’s disease, named after Walter P. Blount, describes a progressive (worsening with time) proximal tibial varus deformity. This is when a child is bow-legged in their lower leg bone or tibia. It occurs in two different age groups – an infantile form that typically develops shortly after the child starts to walk, and an adolescent form. Physiologic bowing is a normal part of the development pattern for newborns and typically resolves by approximately 2 years of age. In younger children with severe bowing or bowing on only one side, it is important to distinguish physiologic bowing from Blount’s disease. This is often done by referral to a pediatric orthopaedist.
Cause
Blount’s disease results from a disturbance of the medial (inner) aspect of the growth plate (physis) in the upper portion of the tibia at the knee, resulting in progressive bowing of the leg.
Infantile Blount’s disease occurs in children younger than 3 years old. Although the underlying cause is not fully known, being overweight may increase the forces seen at the part of the growth plate that is diseased and may predispose to infantile Blount’s disease, particularly in those who begin walking at an earlier age. The cause of adolescent Blount’s disease is also not completely known. It is, however, more common in males and in the setting of obesity.
Description
The classic findings of infantile Blount’s disease include a leg that is bowed due to an angulation in the upper part of the tibia. The growth plates of the tibia and fibula near the knee are diseased and appear abnormal on plain radiographs or x-rays. Your physician may measure certain angles on the images to try to determine if your child has infantile Blount’s disease versus physiologic bowing. Sometimes infantile Blount’s disease is so severe that the growth plate cannot function on one side because bone has formed across it.
The adolescent form of Blount’s disease occurs when a patient is older. It more commonly affects one leg but also may involve both legs. It is associated with obesity and thought to be related to stress on the growth plate. It is often associated with associated deformities of the knee such as a procurvatum deformity of the proximal tibia (a deformity that makes it hard to fully straighten the knee) and an internal tibial torsion (internal twist of the tibia which makes the foot point inward while walking). There may also be an associated deformity of the distal femur (thigh bone above the knee) or distal tibia (shin bone at the ankle).
Doctor Examination
The orthopaedist will take a detailed history including asking about family history of bowed legs. Possible referral for a full medical workup and evaluation by a pediatrician may be placed. A physical examination will include an examination of the legs including range of motion of the hip, knee, and ankle, the alignment of the limbs and examination for a possible leg length differences. The doctor will observe how your child walks. Radiographs or x-rays of the legs will be obtained to look at the growth plates involved and a potential difference in leg lengths. The radiographs will also help rule out other causes of bow legs such as skeletal dysplasias, metabolic diseases such as Rickets, trauma or infection and other less common underlying diagnoses. MR imaging (MRI) may be ordered in some cases to gather more information about the health of the proximal tibial growth plate.
Nonsurgical Treatment
The treatment options and recommendations depend upon many factors such as the age of the patient, the severity of the growth plate disease and the magnitude of the lower extremity deformity.
For children under age 3 with a mild stage of Blount’s disease, bracing maybe recommended. The braces may need to be adjusted as your child grows and as the alignment of the leg changes. Close follow-up during the bracing period is essential as continued progression of the Blount’s disease despite bracing may warrant surgical intervention.
The nonsurgical management of adolescents with Blount’s disease focuses more on the full medical evaluation and management of other medical problems. In many cases, weight management may be indicated as well as evaluation of the patient’s metabolic status, pulmonary status, possible obstructive sleep apnea and cardiovascular health. However, surgery is necessary to treat the bony deformity.
Surgical treatment
There are a number of operative treatment strategies for both the infantile and adolescent forms of Blount’s disease.
Guided growth
One option of treating Blount’s disease in some patients is with a more minimally invasive procedure. The technique involves temporarily tethering the lateral (outside) aspect of the growth plate in order to allow the medial (inside) part of the growth plate to correct the bow legged deformity over time. Plate and screw constructs are most often utilized, although staples or screws are sometimes preferred. On occasion the tethering is done in a permanent fashion. This technique relies upon the medial or inner part of the growth plate being healthy enough to grow. This technique also fails to address other components of the deformity that may be seen in Blount’s disease such as an internal tibial torsion (twisting deformity) or a deformity in the sagittal plane (deformity looking from the side, generally with the inability to full straighten the knee).
Bar Resection
In younger children occasionally the growth plate cannot function properly because a bar of bone as formed across it. In these instances it may be best to remove that bar of bone, and the void is generally filled with fat or cement. This may be done in combination with an osteotomy (described below).
Osteotomy
For children with advanced stages of infantile Blount’s disease, an osteotomy (bone cut) of the proximal tibia and possibly also the fibula is indicated to realign the lower extremity and unload the diseased portion of the proximal tibial growth plate.
An osteotomy can either be acutely or gradually corrected. If it is acutely corrected, it is held in place with pins or a plate and/or a cast such that the lower extremity is corrected in the operating room and then held in place to heal. The limitations of this strategy may include the size of the deformity, particularly in older children and the limits of the nerves, blood vessels and soft tissues of the leg.
If an osteotomy is gradually corrected, an external fixator such as a hexapod frame is placed at the time of surgery. The image shown below is an example of a hexapod external fixator used to correct a severe deformity associated with adolescent Blount’s disease. An advantage to gradual correction with a hexapod external fixator is the ability to add a component of lengthening in the setting of a leg length discrepancy.
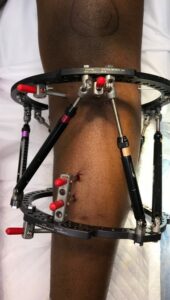 Physiolysis (“stopping” a growth plate)
Physiolysis (“stopping” a growth plate)
For children in whom the medial portion of the proximal tibial growth plate is damaged to the point that even with a realignment or straightening procedure it is not able to grow, it may be necessary to stop the remainder of the proximal tibial growth plate in order to prevent the deformity from recurring one or multiple times. This intervention may bring about a significant discrepancy in leg lengths which may require halting the growth of an unaffected opposite leg or may involve lengthening procedures.
Hemiplateau elevation
In children, young adults or older adults in whom the deformity is very severe, it may be recommended to perform an intra-articular (inside the joint) osteotomy of the proximal tibia to elevate the medial portion of the proximal tibia. This is a special type of osteotomy where the shape of the joint is changed. A dynamic assessment of the knee joint stability and/or assessment with an arthrogram (injection of dye which is visible on x-rays into the joint) to outline the cartilaginous elements of the joint may help determine the indications for this procedure. A hemiplateau elevation may be performed in conjunction with additional treatment options.
Complications of surgery
It is important to acknowledge that undergoing surgical intervention to treat a severe lower extremity deformity incurs risk. The deformity may recur and/or other complications may ensue. Your surgeon will discuss the risks with you and your family and ways of preventing and addressing these risks.